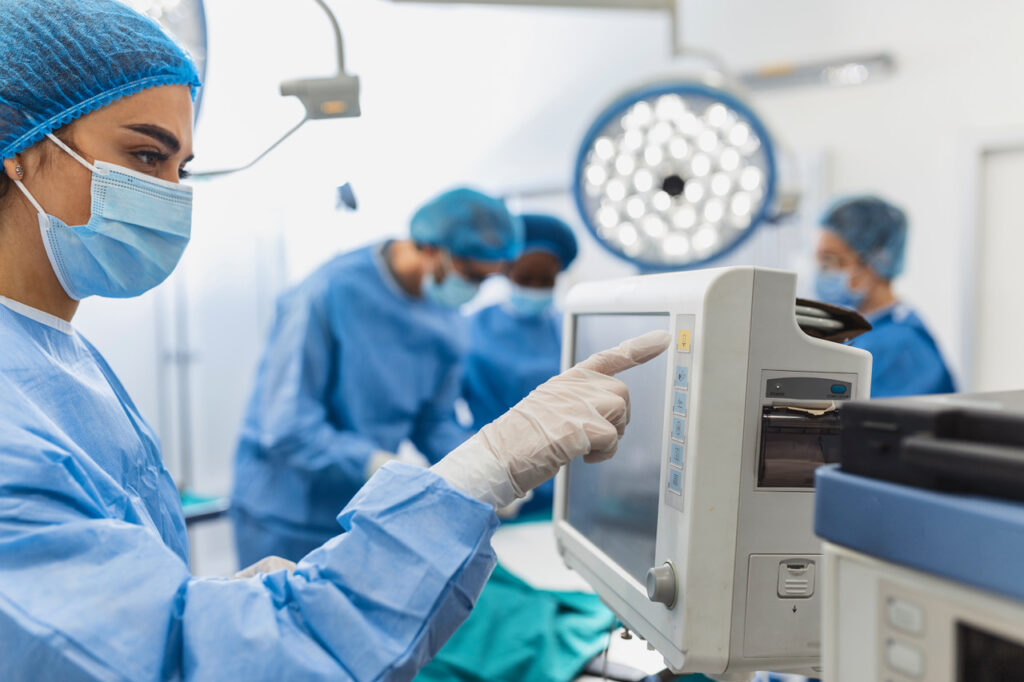
On-pump vs. off-pump coronary artery bypass grafting (CABG)
Off-pump CABG avoids complications that can arise with the cardiopulmonary bypass and manipulation of the aorta. Thus, off-pump CABG appears to provide superior short-term outcomes specifically by reducing the risk of perioperative stroke, renal dysfunction, blood transfusion, wound infection, respiratory failure, atrial fibrillation, ventilation time, and ICU and hospital length of stay.1 However, the trade-off may be reduced graft patency and increased risk of cardiac re-intervention and death.1 While the literature is a bit muddled,2,3 on-pump, or traditional, CABG seems to be associated with better long-term outcomes than off-pump CABG.4,5 Despite these trade-offs and a fair bit of controversy6, off-pump CABG is a valid approach for select (usually high risk) patients, especially when precise and complete revascularization is prioritized.
Risk factors for perioperative myocardial infarction following CABG are unclear
Unfortunately, it is still clinically challenging to determine which patients are best suited to off-pump CABG. One of the major barriers to accurate risk assessment is the high rate of perioperative myocardial infarction associated with CABG, either on-pump or off-pump. Perioperative MI (Type 5) may occur in as many as 3 in 10 patients who undergo CABG.7 Sadly, this risk of perioperative MI makes the risk-based decision between on-pump and off-pump CABG even more difficult.
Obstructive sleep apnea is an independent risk factor for MI following off-pump CABG
A recent study prospectively followed 147 consecutive patients at a single hospital scheduled to have off-pump CABG.8 In addition to the extensive bloodwork required before surgery, each study participant underwent portable cardiorespiratory polygraphy with a device similar to one used for at-home sleep apnea testing. This testing identified 62 patients with obstructive sleep apnea (42.2% of the cohort). Of the 147 patients who then had off-pump CABG, 24 were diagnosed with perioperative MI, 17 patients had obstructive sleep apnea, and 7 patients did not, which was a significant difference (P = 0.002). Furthermore, multivariate logistic regression revealed that apnea-hypopnea index (AHI, a measure of sleep apnea severity) was significantly associated with perioperative MI following off-pump CABG. Similar associations were discovered for high-sensitivity c-reactive protein (hs-CRP) and SYNTAX (SYNergy between PCI with TAXUS and Cardiac Surgery9,10) score, which were also independent risk factors for patients with perioperative MI after off-pump CABG.8
Possible mechanistic links between obstructive sleep apnea and perioperative MI
The authors of this prospective study speculated on the pathophysiologic mechanisms that would undergird their clinical findings. They pointed out that patients with obstructive sleep apnea showed signs of increased systemic inflammation, which promote the formation of atheromatous lesions, including within coronary arteries.11,12 Certainly the strong association with hs-CRP levels seen in the current study would support that putative link. Furthermore, patients with obstructive sleep apnea have enhanced platelet activation and rates of aggregation13 and diminished fibrinolytic capacity.14
The role of CPAP for CABG patients with obstructive sleep apnea
Indirect evidence suggests CPAP treatment for patients with obstructive sleep apnea could have a beneficial effect on this patient population. CPAP appears to correlate with lower levels of inflammation,15 improvements in markers of atherosclerosis,16 and reduced coagulability.17 Cassar et al. (32) found that screening for and treating obstructive sleep apnea with CPAP decreased cardiac death in patients who underwent percutaneous coronary intervention (PCI). Admittedly, these data do not get to the heart of whether CPAP can reduce the apparent increased risk of perioperative MI in patients with obstructive sleep apnea; prospective interventional studies are needed for that. However, until that question is answered, CPAP treatment poses little risk and potentially substantial reward for these individuals.
Practice implications for cardiologists and cardiothoracic surgeons
Now that obstructive sleep apnea, hs-CRP, and SYNTAX score are known independent risk factors for perioperative MI after off-pump CABG, these variables should be quantified prior to surgery and factored into the overall risk assessment. Since SYNTAX score is calculated with an algorithm based on angiography results—available in all patients destined for CABG—determining this value adds negligibly to the workflow. The same is true for the hs-CRP blood assay. While formal polysomnography could add substantially to pre-surgical planning, at-home sleep apnea testing is relatively inexpensive and convenient for patients. Surgeons can order the study for patients directly and the results are interpreted remotely by a sleep medicine specialist. Perhaps most importantly, at-home sleep apnea testing has comparable sensitivity and specificity with polysomnography or in laboratory sleep study testing.18-20 In fact, home sleep apnea testing was used in the current study.8 Thus, cardiologists and cardiothoracic surgeons can feasibly integrate these three critical risk factor assessments into every patient’s pre-CABG surgical evaluation workflow.
References
1. Puskas JD, Martin J, Cheng DC, et al. ISMICS Consensus Conference and Statements of Randomized Controlled Trials of Off-Pump Versus Conventional Coronary Artery Bypass Surgery. Innovations (Phila). 2015;10(4):219-229. 10.1097/IMI.0000000000000184
2. Diegeler A, Borgermann J, Kappert U, et al. Off-pump versus on-pump coronary-artery bypass grafting in elderly patients. N Engl J Med. 2013;368(13):1189-1198. 10.1056/NEJMoa1211666
3. Lamy A, Devereaux PJ, Prabhakaran D, et al. Five-Year Outcomes after Off-Pump or On-Pump Coronary-Artery Bypass Grafting. N Engl J Med. 2016;375(24):2359-2368. 10.1056/NEJMoa1601564
4. Smart NA, Dieberg G, King N. Long-Term Outcomes of On- Versus Off-Pump Coronary Artery Bypass Grafting. J Am Coll Cardiol. 2018;71(9):983-991. 10.1016/j.jacc.2017.12.049
5. Shroyer AL, Hattler B, Wagner TH, et al. Five-Year Outcomes after On-Pump and Off-Pump Coronary-Artery Bypass. N Engl J Med. 2017;377(7):623-632. 10.1056/NEJMoa1614341
6. Gaudino M, Angelini GD, Antoniades C, et al. Off-Pump Coronary Artery Bypass Grafting: 30 Years of Debate. J Am Heart Assoc. 2018;7(16):e009934. 10.1161/JAHA.118.009934
7. Thielmann M, Sharma V, Al-Attar N, et al. ESC Joint Working Groups on Cardiovascular Surgery and the Cellular Biology of the Heart Position Paper: Perioperative myocardial injury and infarction in patients undergoing coronary artery bypass graft surgery. Eur Heart J. 2017;38(31):2392-2407. 10.1093/eurheartj/ehx383
8. Fan K, Gao M, Yu W, et al. Obstructive Sleep Apnea Increases the Risk of Perioperative Myocardial Infarction Following Off-Pump Coronary Artery Bypass Grafting. Front Cardiovasc Med. 2021;8:689795. 10.3389/fcvm.2021.689795
9. Farooq V, Girasis C, Magro M, et al. The CABG SYNTAX Score – an angiographic tool to grade the complexity of coronary disease following coronary artery bypass graft surgery: from the SYNTAX Left Main Angiographic (SYNTAX-LE MANS) substudy. EuroIntervention. 2013;8(11):1277-1285. 10.4244/EIJV8I11A196
10. Ishiwata S, Tomita Y, Ishiwata S, Narui K, Daida H, Kasai T. Association between Obstructive Sleep Apnea and SYNTAX Score. J Clin Med. 2020;9(10). 10.3390/jcm9103314
11. Ryan S. Mechanisms of cardiovascular disease in obstructive sleep apnoea. J Thorac Dis. 2018;10(Suppl 34):S4201-S4211. 10.21037/jtd.2018.08.56
12. Ryan S, Taylor CT, McNicholas WT. Selective activation of inflammatory pathways by intermittent hypoxia in obstructive sleep apnea syndrome. Circulation. 2005;112(17):2660-2667. 10.1161/CIRCULATIONAHA.105.556746
13. Bokinsky G, Miller M, Ault K, Husband P, Mitchell J. Spontaneous platelet activation and aggregation during obstructive sleep apnea and its response to therapy with nasal continuous positive airway pressure. A preliminary investigation. Chest. 1995;108(3):625-630. 10.1378/chest.108.3.625
14. Rangemark C, Hedner JA, Carlson JT, Gleerup G, Winther K. Platelet function and fibrinolytic activity in hypertensive and normotensive sleep apnea patients. Sleep. 1995;18(3):188-194. 10.1093/sleep/18.3.188
15. Yokoe T, Minoguchi K, Matsuo H, et al. Elevated levels of C-reactive protein and interleukin-6 in patients with obstructive sleep apnea syndrome are decreased by nasal continuous positive airway pressure. Circulation. 2003;107(8):1129-1134. 10.1161/01.cir.0000052627.99976.18
16. Drager LF, Bortolotto LA, Figueiredo AC, Krieger EM, Lorenzi GF. Effects of continuous positive airway pressure on early signs of atherosclerosis in obstructive sleep apnea. Am J Respir Crit Care Med. 2007;176(7):706-712. 10.1164/rccm.200703-500OC
17. Phillips CL, McEwen BJ, Morel-Kopp MC, et al. Effects of continuous positive airway pressure on coagulability in obstructive sleep apnoea: a randomised, placebo-controlled crossover study. Thorax. 2012;67(7):639-644. 10.1136/thoraxjnl-2011-200874
18. Hedner J, White DP, Malhotra A, et al. Sleep staging based on autonomic signals: a multi-center validation study. J Clin Sleep Med. 2011;7(3):301-306. 10.5664/JCSM.1078
19. Hedner J, Pillar G, Pittman SD, Zou D, Grote L, White DP. A novel adaptive wrist actigraphy algorithm for sleep-wake assessment in sleep apnea patients. Sleep. 2004;27(8):1560-1566. 10.1093/sleep/27.8.1560
20. Kasai T, Takata Y, Yoshihisa A, et al. Comparison of the Apnea-Hypopnea Index Determined by a Peripheral Arterial Tonometry-Based Device With That Determined by Polysomnography- Results From a Multicenter Study. Circ Rep. 2020;2(11):674-681. 10.1253/circrep.CR-20-0097
