By Gilad Glick | September 6, 2017
Why has sleep breathing management not integrated into cardiology care pathway?
In my previous article, I briefly mentioned the increased awareness and the broad acceptance of the role of Sleep Apnea in Cardiac disease and the main studies and scientific statements published by the ESC, AHA and ACC which were the driver behind the American Sleep Academy “Sleep Apnea Hurts Hearts” campaign.
The question remaining is:
If the link between Sleep Apnea and several main cardiovascular diseases such as Atrial Fibrillation and Hypertension has been broadly accepted – why DO most heart patients remain undiagnosed and majority of cardiologist are not integrating this factor into their care pathway?
There are two main barriers that we hear about from practitioners:
The first obstacle is awareness of cardiologists and their patients about how prevalent Sleep Apnea is among cardiology patients and the fact that most will not be visually detected. Most cardiologists “eyeball” patients to assess obvious signs of sleep apnea such as a thick neck, visually high BMI, chronically blocked nose etc.
This results in significant underdiagnosis of sleep apnea as demonstrated in a recent study conducted in Montefiore medical center (New York) by Dr. Wharton and Dr. Zaremski. Their conclusion was that systematic and broad screening is recommended in cardiology clinics, with 84% of their patients screened positive for sleep apnea, while BMI was a poor predictor of screening results.
The second obstacle lies in the dynamics of referring a patient to a sleep medicine physician: to start with, cardiology patients are pre-occupied with their heart condition, and do not understand the link between their Sleep Apnea and their heart. If not given a motivational explanation by the cardiologist or pressed hard to show up at the sleep doctor – most will not make this extra effort this requires.
Furthermore, when patients finally overcome this obstacle and wish to take a sleep study, they encounter the lack of sufficient sleep certified physicians, resulting in inconvenient waiting times, sometimes reaching months combined with geographical accessibility limitations driven by the tendency to diagnose simple OSA with full in-lab polysomnography (PSG) as first line procedure which has a host of barriers imbedded in it.
For example, more and more medical insurers will require Home Sleep Apnea Test (HSAT) before authorizing PSG. Sleep physicians, preferring PSG – require the patient to undergo 2 procedures or debate the insurance. Not an insignificant portion of the patients refuse to undergo in-lab PSG because they are worried about being hospitalized or fear the financial impact of the co-pay. Sleeping at a sleep lab is also not an experience people look forward to.
Harnessing the simplicity of home sleep tests
As a result, the integration between cardiology and sleep needs to be done differently. Home sleep tests, which revolutionized sleep medicine and made sleep studies available to all patients, whether they lived far, had a disability or simply liked sleeping in their own beds – has the promise to enable the cardiology patient population to easily manage their sleep. By either moving the point of dispatch to Cardiology or even to direct shipment – just like Amazon did with retail.
How do we solve these challenges?
Recently Itamar Medical launched the Total Sleep Solution program that has all the components necessary to successfully integrate Sleep medicine into Cardiology patient care. It has:
(A) Cardiology oriented screening tools – combined with patient education materials to achieve efficient accessibility for all patients while maintaining a seamless and pleasant patient experience.
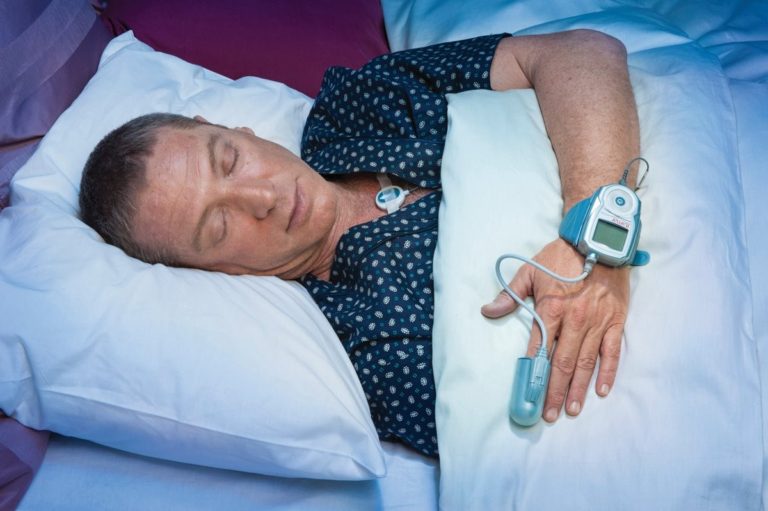
(B) Unique Home Sleep Testing – Enabling Technology with the WatchPAT home sleep test which offered unparalleled simple user experience, requiring only a finger sensor and a watch instead of all the cumbersome home sleep tests available. It’s FDA cleared, listed as technically adequate in the AASM guidelines for HSATs[1] and fully reimbursed*
(C) Remote sleep expert interpretation – Cloud based technology that enables immediate transmission of the test report to a sleep specialist for interpretation and diagnosis, because we at Itamar understand cardiologists are not interested in practicing sleep or pulmonary medicine and
(D) Connection to sleep apnea management service providers of high quality that understand the standards Cardiologists are expecting and help ensure patient compliance and adherence.
To learn more about our comprehensive customizable solutions, you may always contact your local Itamar Sales Representative or leave your details here:
[1] Kapur VK, et al. 2017 “Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline.”J Clin Sleep Med. 13(3):479–504.
*Please verify with your insurance mix as local policies varies
