
On December 1st, 2020, the Centers of Medicare and Medicaid Services (CMS) issued revisions to the Physician Fee Schedule (PFS) which outlines payment policies, rates, and quality provisions for services provided under Medicare.2
The goal of the CMS revision was to prioritize primary care, chronic disease management and telehealth services. The revisions were designed to:2
- Allow non-physician practitioners to provide care that they are licensed and trained to perform
- Expand coverage for telehealth services adding 144 services that will be covered through the end of COVID-19 pandemic
- Increase payment rates for in-office and outpatient face-to-face evaluations and management (E/M) visits for chronic conditions
Then, on December 29th, 2020, some additional adjustments were made that amounted to the following items:1
- Provided a 3.75% increase in MPFS payments for CY 2021
- Suspended the 2% payment adjustment (sequestration) through March 31, 2021
- Reinstated the 1.0 floor on the work Geographic Practice Cost Index through CY 2023
- Delayed implementation of the inherent complexity add-on code for evaluation and management services (G2211) until CY 2024
Q: What does that mean for HSAT reimbursement?
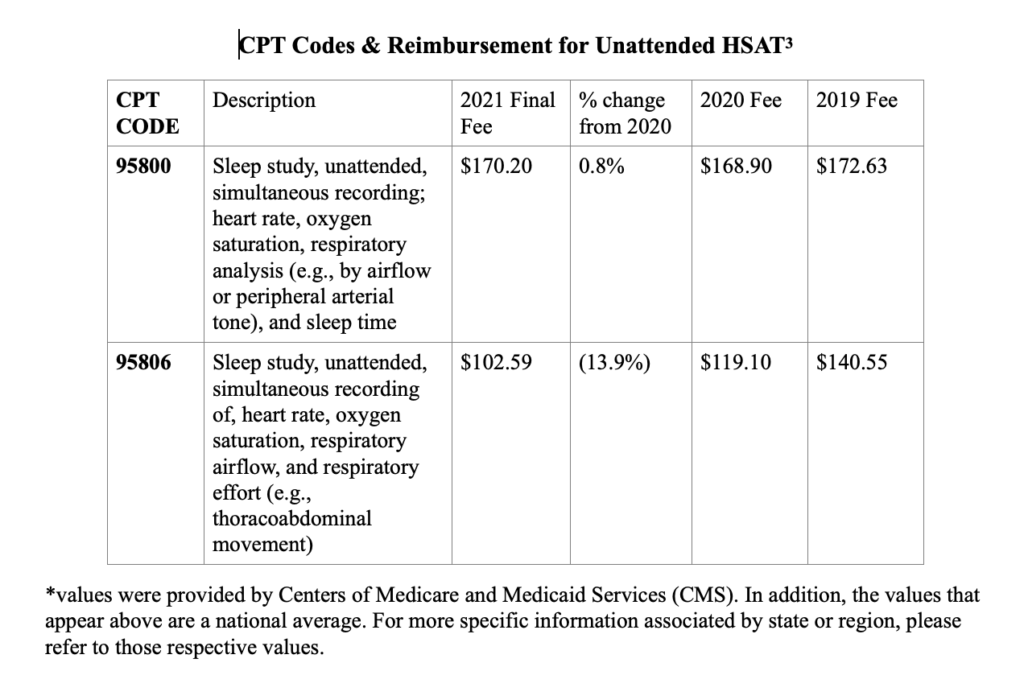
A: These revisions led to reimbursement changes for different services and procedures, including home sleep apnea testing (HSAT). HSAT devices that include sleep time, such as the WatchPAT® Home Sleep Apnea Tests , saw an increase in the reimbursement level while traditional airflow tests without sleep time saw a decline in reimbursement.
Q. Do Medicare and third party payers have any restrictions on who can bill for HSAT?
A: Yes. Medicare Administrative Contractors (MACs) require that physicians who interpret the sleep study have a sleep certification issued by specific specialty boards, or be an active member of an accredited sleep center or laboratory. Some MACs also require physicians that provide the sleep study to be credentialed. Check the LCD of your MAC for their requirements. Medicare also restricts durable medical equipment suppliers from providing any component of sleep testing. Third party payers make autonomous decisions in the development of their medical policies and the limitations they set. While some third party payers include sleep certification or accreditation requirements for HSAT in their policies, most do not. Please check payer policies for applicable limitations.
Q. How often can HSAT be performed and qualify for reimbursement?
A: Payers vary on the number of sleep studies that are considered medically necessary per year. Most payers allow two sleep studies per year unless it is medically necessary to repeat a study. It is recommended to seek prior authorization if the payer’s established frequency limitation is exceeded.
Q. How many consecutive nights of study may be performed and reimbursed?
A: Medicare and third party payers state that if you perform two or three nights of study it will only be reimbursed as one night of study. Third party payers may reimburse more than one night of study depending on your specific contract.
For more information about the CMS decision, visit the CMS website. And for additional questions regarding reimbursement with the Watch PAT® Home Sleep Apnea Test download our 2021 Reimbursement Guide.
References:
- Physician Fee Schedule. CMS. https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/PhysicianFeeSched. Accessed February 26, 2021.
- Press release Trump Administration Finalizes Permanent Expansion of Medicare Telehealth Services and Improved Payment for Time Doctors Spend with Patients. CMS.gov. https://www.cms.gov/newsroom/press-releases/trump-administration-finalizes-permanent-expansion-medicare-telehealth-services-and-improved-payment.
- Sleep Medicine Codes. AASM.org. https://aasm.org/clinical-resources/coding-reimbursement/sleep-medicine-codes/. Published December 14, 2018. Accessed January 31, 2021.
- Physician Fee Schedule Search. CMS.gov Centers for Medicare & Medicaid Services. https://www.cms.gov/apps/physician-fee-schedule/search/search-criteria.aspx. Accessed January 31, 2021. Published December 1, 2020. Accessed January 31, 2021.
