By Efrat Magidov
Abdominal aortic aneurysm (AAA) is a potentially life-threatening condition that may be exacerbated by Obstructive Sleep Apnea (OSA) which has been verified as an independent causal factor in the pathogenesis of hypertension and vascular dysfunction. More specifically, several pathomechanisms have been suggested to account for the potential adverse effect of OSA on AAA:
- The intrathoracic pressure changes leading to shear stress on artery walls;
- Intermittent hypoxia leading to oxidative stress, sympathetic stimulation, and possibly atherosclerosis;
- Arousal-induced sympathetic activation inducing subsequent repetitive blood pressure surges and chronic hypertension.
The attempts to link obstructive sleep apnea (OSA) to AAA are based on early studies of patients with Marfan’s syndrome. In the early 90s, it was first suspected that OSA may have deleterious effects on the aorta in Marfan’s syndrome patients. Later researchers demonstrated higher prevalence of OSA in those patients and described a correlation between OSA severity (as measured by the apnea-hypopnea index (AHI)) and aortic root diameter (r=0.5, p<0.001). In a follow-up longitudinal study of 44 Marfan’s syndrome patients, only subjects with OSA developed an aortic event (after a median follow-up time of 29 months). Although the relative risk of OSA was not successfully assessed due to the small sample size, this remains the only longitudinal study which investigated the effect of OSA on the aorta by means of events (rather than disease parameters).1
Several cross-sectional studies on the general population found a positive association between the aortic root diameter and OSA severity.
Interestingly, simulating OSA in healthy volunteers with the use of Muller’s maneuver induced considerable changes in both blood pressure and proximal aortic diameter and area, probably due to increased aortic dilatory pressures. Observational studies have consistently reported that OSA is highly prevalent among patients with AAA. In one such study by Mason and colleagues, 127 patients (11 women, mean age 67.9±6) with an abdominal aortic measurement greater than or equal to 30 mm were examined. Home sleep monitoring was used to assess OSA presence in terms of ODI (>4%) and AHI. Approximately 40% of the patients were found to have an ODI greater than 10 per hour, representing a 5-fold greater incidence than in a comparable normal population. Similarly, 29% of the patients had AHI greater than 15, almost 2 times higher than the normal prevalence values.
These results correspond to other studies demonstrating up to 60% OSA presence in AAA patients which is significantly higher than the estimated prevalence of 17% in the general population. Importantly, subjective reports did not reveal a correlative sleepiness, suggesting that daytime sleepiness is not suitable for detecting OSA in AAA patients.
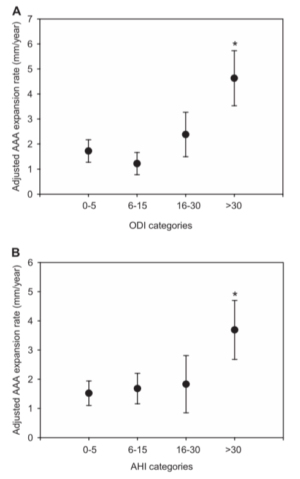
The researchers went on to examine whether OSA can explain occurrences of AAA expansion. They compared the AAA diameter of two duplex scans; one from the recruitment phase and another before the sleep study (median follow-up time was 18 months). Severe OSA, represented by ODI and AHI greater than 30, was found to be significantly associated with a high AAA expansion rate (ODI- 2.9 mm per year, p=0.009; AHI- 2.2 mm per year, p=0.043 – Figure 1). These results were derived after adjustment to cardiovascular risk factors and medication use, and therefore represent OSA relative risk. The presence of correlation only at severe OSA suggests a threshold effect rather than a simple linear dose–response relationship between OSA severity and AAA expansion rate.2
Through these studies, it is becoming clear that successful diagnosis of OSA in AAA patients can be an important factor in managing the risk of lethal aortic complications. Future studies will hopefully examine the potential beneficial effects of OSA-treatment on AAA. WatchPAT, a home sleep apnea test device, is a simple, accurate and reliable tool for OSA diagnosis. You may learn more about WatchPAT and our comprehensive “Total Sleep Solutions” for Cardiology practices at www.cardiosleepsolutions.com
sources:
- Gaisl, T., Bratton, D. J., & Kohler, M. (2015). The impact of obstructive sleep apnoea on the aorta. European Respiratory Journal, 46(2), 532-544.
- Mason, R. H., Ruegg, G., Perkins, J., Hardinge, M., Amann-Vesti, B., Senn, O., … & Kohler, M. (2011). Obstructive sleep apnea in patients with abdominal aortic aneurysms: highly prevalent and associated with aneurysm expansion. American journal of respiratory and critical care medicine, 183(5), 668-674.
